Seminal Vesicle: Everything a Man Needs to Know

Table of Contents
- Seminal tract: Overview
- Seminal vesicle: Function
- Seminal tract infection, and who’s prone to it?
- Seminal tract infection symptoms: Recognising male genital tract issues
- Diagnosing seminal vesicle issues: Methods
- Treating seminal tract infection
- How does seminal vesicle function get affected by surgical treatment?
- How to prevent seminal tract infection symptoms?
- Conclusion
- FAQs :
The seminal vesicle is a paired accessory gland above the prostate gland. It contributes significantly to semen formation (fructose, prostaglandins), ensuring the ejaculatory duct remains lubricated for smooth insemination (transfer of sperm during copulation).
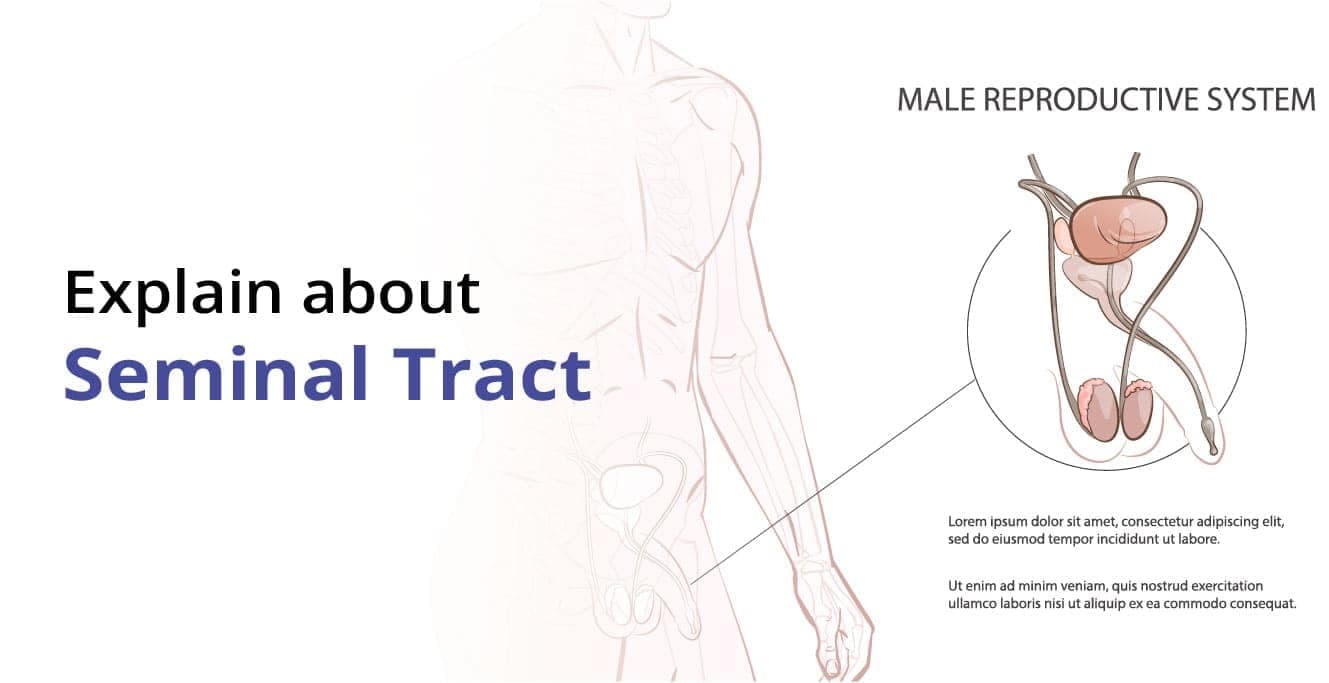
The seminal tract comprises seminiferous tubules, epididymis, vas deferens and the ejaculatory tract. It transfers the matured sperms from the testicular lobules to the tip of the penis and forth into the cervical region during copulation.
Unprotected sex can lead to seminal tract infections like AIDS and chlamydia.
Why Choose Us?
 120+ IVF Experts
120+ IVF Experts 1,40,000+ Couples Helped
1,40,000+ Couples Helped
Seminal tract: Overview
The seminal vesicles represent vacuolar muscles that have exocrine properties. It lies at the tip of the penis, playing a crucial role in semen formation. Also known as seminal or vesicular glands, they look like sacs and lie behind the urinary bladder.
The seminal tract carries the sperm and channels the secretion from the vesicles, bulbourethral gland and the prostate, leading to semen analysis.
The ejaculatory duct or male urinogenital tract is also a part of the seminal tract. When it’s affected, it leads to insufficient sperm production lowering fertility chances.
Seminal vesicle: Function
The role of the seminal vesicle is unanimous as an accessory organ in healthy sperm production. It includes:
- Acting as a temporary site of storage for sperms when insemination doesn’t take place
- Forms nearly the bulk (70% to 80%) of the semen volume
- Imparts an alkaline pH to the outgoing semen (neutralising acidic pH present in the vagina)
The seminal vesicle secretes the following compounds that provide characteristic properties to the milky white semen. It includes:
- Alkaline fluid maintains a favourable pH to counter intravaginal acidic conditions.
- Fructose acts as an energy reserve to enhance travelling sperms reach the junction of fertilisation.
- The presence of P, K, and Ca maintains the vigour and vitality of the sperms (whiplash movement).
- Seminal glands secrete prostaglandins, which provide a physiological barrier to the sperms. It also enhances their motility and penetration capacity.
- Semen contains proteins like semenogelin, which provides a gel-based protective covering to the sperms.
Seminal tract infection, and who’s prone to it?
The seminal tract is unique to the male urinogenital system. It can act as a medium to spread among women if the individual is an STI carrier.
The pathogen affecting the male genital tract also affects the underlying organs (prostate) and can inflict far-extending damage to the testis.
It’s no coincidence that sexually transmitted infection shares the same acronym with seminal tract infection in men. Individuals include:
- Men with multiple pleasure partners (homosexuals and heterosexuals)
- Practising unprotected sexual intercourse with strangers
- Underlying pathogens like bilharzia and filariasis cause fluid accumulation affecting the testicular region.
- Seminal vesicle inflammation (vesiculitis)
- Inguinal hernia
- Vesicular agenesis
- Cyst formation (renal calculi, polycystic kidney, diabetes and cystic fibrosis)
Seminal tract infection symptoms: Recognising male genital tract issues
If you feel uncomfortable while passing urine daily or report unnatural substances like blood, minute renal stones and a burning sensation, it might show a potential seminal tract infection. Symptoms include:
- Feeling pain during urination and the same during copulation
- Presence of blood when passing urine (haematuria) and the same with seminal fluid (haematospermia)
- Constant pain and underlying burning sensation after passing urine
- Reduced seminal volume during insemination (chances of infertility)
- Unexplained pain limited to the male pelvic region (penile, scrotal and lower abdomen)
The highlighted symptoms could show seminal tract issues, including further complicated health anomalies like prostate cancer advancing undetected.
Diagnosing seminal vesicle issues: Methods
Visit your physician or urologist specialist if you experience one of the mentioned symptoms over a couple of weeks. It includes mechanical and diagnostic examinations to evaluate the nature of seminal tract infection. Methods include:
- Urine culture (urinalysis)
- 3D ultrasound of the pelvic region (transrectal USG)
If these examinations cannot spot the underlying issue, additional methods include:
- Computed tomography scan (CT)
- Magnetic resonance imaging scan (MRI)
- Positron emission tomography scan (PET)
Treating seminal tract infection
Both drug therapy and minimally invasive technique can effectively treat underlying seminal tract issues. Patients with STIs and pathogenic growth in the male urinogenital tract require antibiotics (cefixime), and a disciplined routine is necessary to prevent further infection.
If the underlying issues affect the seminal vesicle or block the natural transport of seminal fluid, a surgical response is the most effective choice. The patient may undergo:
- Paracentesis (an invasive technique to use a surgical needle for extracting fluid accumulation around the penile base)
- Using laparoscopy to neutralise and remove cyst-like formation in the intrauterine tract
- Patients having prostate carcinoma undergo prostatectomy; it removes the prostate gland and the associative glands surrounding it
How does seminal vesicle function get affected by surgical treatment?
The seminal vesicle, bulbourethral and prostate gland play a crucial role in semen formation. If either organ gets removed surgically owing to health anomalies, here’s the list of potential side effects:
- Intrauterine bleeding
- Reduced or little seminal volume
- Drying of the seminal tract (absence of lubrication)
- Facing erectile dysfunctional syndrome
- Urinary discomfort
- Unable to voluntary control urination (urine incontinence)
- Risks of intrauterine infection
How to prevent seminal tract infection symptoms?
Most seminal tract issues develop from casual behaviour, leading to underlying illness. Here’s how you can prevent it:
- Advocate safe sexual practices (take adequate protection when having sex with strangers)
- Undergo health checkups to find out whether you are a carrier of the potential urinogenital illness
- Abstain from substance abuse (tobacco); it’s a proven trigger for prostate cancer
- Control your BMI and physiological vitals (preventing adipose tissue deposition around the abdomen); it affects the natural function of the seminal tract in men
We take care of you
Begin Your Treatment Journey with Confidence


No Cost EMI

Dedicated Insurance Support
Conclusion
The seminal tract and a pair of healthy seminal vesicles have an immense role in maintaining Male Infertility and natural urination. Ignoring pelvic discomfort or contracting STIs affects both testicular functions and urine formation.
Patients having a parental history of urinogenital issues should take preventive measures early to prevent infection. Just like women are vulnerable to UTIs, without an early treatment of seminal tract infection may lead to complete sterility, let alone develop issues like prostate cancer.
CTA: Facing penile discomfort? Producing low seminal volume during copulation could show signs of seminal tract issues. Take a free consultation with our experienced urologists at your nearest Birla Fertility and IVF clinic today to learn more about your condition.
FAQs :
1. What role does the seminal vesicle play in male fertility?
The seminal vesicle is the chief contributor to seminal fluid formation. The sperm cannot travel independently during insemination without necessary seminal volume.
2. How long is the seminal vesicle?
The seminal vesicle measures around 10 cm (uncoiled), while its 3-5 cm and has a diameter of 1 cm when coiled.
3. Why seminal tract is vital for male fertility?
The seminal tract is vital for carrying sperms from the testis to the urethra through the ductus deferens, helping in the formation of semen and transferring the semen to the ejaculatory duct for insemination.
4. What happens upon the removal of the seminal vesicle?
The absence of the seminal vesicle leads to gradual drying of the seminal tract, lacking in seminal fluid and eventually leading to erectile dysfunction and infertility.
Our Fertility Specialists
Related Blogs
To know more
Birla Fertility & IVF aims at transforming the future of fertility globally, through outstanding clinical outcomes, research, innovation and compassionate care.
Had an IVF Failure?
Talk to our fertility experts

 Our Centers
Our Centers