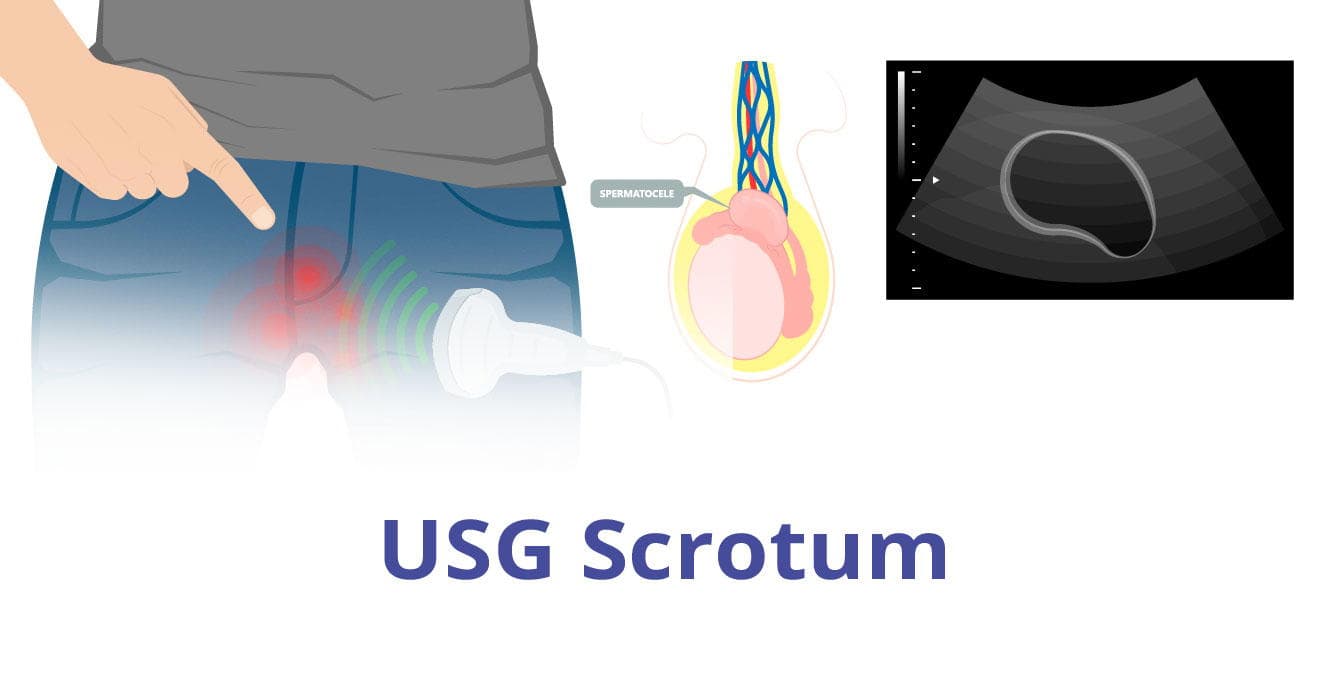
What is the USG Scrotum

USG Scrotum or ultrasonography of the scrotum is a test in which sound waves are used to produce pictures of a male’s testicles and surrounding tissues.
In this process, the testicles, epididymis (tubes immediately next to the testicles that collect sperm), and scrotum are scanned to check for disorders. USG scrotum is a safe and noninvasive procedure.
Why Choose Us?
 120+ IVF Experts
120+ IVF Experts 1,40,000+ Couples Helped
1,40,000+ Couples Helped
Common Uses of the USG Scrotum
A scrotum test is used to look at a variety of scrotal, testicular, or epididymis issues.
In case you feel like you have pain, swelling, or an injury to the testicles or their surrounding areas, a doctor may advise a USG scrotum for:
- Identifying the location and type of mass in the scrotum that you or the doctor feels to be cystic or solid
- Determining the effects of scrotal injuries
- Identifying the underlying reasons for testicular pain or swelling, such as torsion or inflammation
- Analyzing the origin of the problem, such as varicocele
- Searching for the testes’ undescended position
Besides these, some specific uses for a USG scrotum include:
Testing Testicular Lumps
A doctor will prescribe a scrotal check if they have a suspicion about testicular cancer.
This test is used to check whether a lump found in your testicles has the potential of becoming cancerous. The doctor can see the lump’s size and location using ultrasound imaging.
The scans of the USG scrotum can also assist the doctor in determining if the lump is solid or fluid-filled, harmless or malignant.
Finding Testicular Torsion
Torsion of the testicles is a dangerous, excruciating disorder that needs immediate medical intervention. It occurs when the spermatic cord, which nourishes the testicle with blood, twists.
To determine the extent of testicular torsion, you will need to undergo a testicular torsion ultrasound, followed by surgery. Testicular tissue will perish if testicular torsion is not treated with time due to the blood supply being cut off.
Determining Epididymitis
The epididymis is the tightly coiling tube that houses and carries sperm behind the testicles.
Epididymitis happens when this tube gets inflamed. This causes an accumulation of fluid and leads to the formation of a lump or swelling around the testicle.
Epididymitis is usually caused by the direct spread of infection in around 20–40% of cases and causes acute scrotal pain in men.
So, in case you are experiencing scrotal pain, your doctor may recommend that you undergo a USG scrotum test.
Finding Undescended Testicles
Young males are frequently affected by the problem of undescended testicles.
The testicles should normally descend throughout foetal growth from inside the abdomen to eventually outside the body in the scrotum. This typically occurs before delivery, although it can also happen within six months following delivery.
It is critical to see a professional if a boy’s testicles have not descended by the time he is six months old. The professional will recommend a USG scrotum to find the undescended testicles.
In some cases, the scrotum test can be followed by surgery. Typically, the procedure is simple and entails the surgeon lowering the testicles downward so that they sit correctly in the scrotum.
Procedure for the USG Scrotum
A doctor with expertise in testicular ultrasonography will perform the examination. The operator can be a sonographer, urologist, or radiologist. They will let you know what will happen throughout the USG scrotum before the test starts.
For the USG scrotum, you will need to wear a hospital gown and lie face up on a table before inspection. You may also have to shift to one side during the test.
For optimal contact between the skin and the transducer (a hand-held device), the doctor will apply a water-based gel to your scrotum. The gel also makes it possible to slide the transducer smoothly across your skin. It can feel a bit cold, even though it is occasionally warmed up first.
To take pictures of the testicles, the medical practitioner will rock the transducer back and forth over the scrotum. The pressure from the transducer is often very little. However, if there is an injury or oedema in the area, it can feel uncomfortable.
Typically, ultrasonography of the scrotum lasts for about 15–30 minutes and ends with the doctor wiping away the gel from your scrotum. The ultrasound images are processed quickly, and a scrotal ultrasound report is prepared upon assessment and interpretation by a medical professional.
The doctor can discuss your test results of the USG scrotum with you on the same day of the test or in a follow-up appointment.
How Should I Prepare for the USG Scrotum?
You can do the following to prepare for USG scrotum:
- Shave a bit if there is excessive growth of hair down there
- Have a bath before the test to keep the area clean and hygienic
- Don loose-fitting, comfy attire
- Eat and drink plenty of water
USG Scrotal Scan Cost
The USG scrotum test price can be anywhere between Rs. 2500 and 3000. However, if you are registered under a government/university panel, you can get a concessional rate to get the test done.
We take care of you
Begin Your Treatment Journey with Confidence


No Cost EMI

Dedicated Insurance Support
Conclusion
If you have swelling or pain in your scrotum and wish to have a USG of the scrotum performed, you can visit the nearest Birla Fertility and IVF clinic or book an appointment with Dr. Pankaj Talwar.
Birla Fertility and IVF is a top-notch clinic equipped with the latest tools for conducting USG scrotum tests. The doctors at our clinic believe in providing compassionate and top-quality healthcare services.
FAQs:
Is the USG Scrotum Painful?
No, the USG scrotum is not painful. Instead, it is a safe procedure that produces images of the scrotum with the help of sound waves. This helps in knowing whether something unusual is happening inside your scrotum and testes.
Does Ultrasound Affect Sperm?
According to a study, semen samples of males were collected after they had undergone ultrasounds, and it was found that there was a 40% reduction in sperm motility. So, not one, but having frequent ultrasounds does affect sperm health to an extent.
What Is the Gel Used in Ultrasounds?
The gel used in ultrasounds is composed of propylene glycol (a synthetic chemical frequently found in culinary, hygiene, and cosmetic goods) and water. The gel is thick and sticky. This makes it static and possible to spread across the skin without having to worry about it spilling or running off.
Can Ultrasound Burn Your Skin?
No, ultrasounds can’t burn your skin. Though having an ultrasound can make your skin dry and flaky or leave behind residue that may be greasy or sticky.
Our Fertility Specialists
Related Blogs
To know more
Birla Fertility & IVF aims at transforming the future of fertility globally, through outstanding clinical outcomes, research, innovation and compassionate care.
Had an IVF Failure?
Talk to our fertility experts

 Our Centers
Our Centers Select City
Select City