Endometrial Hyperplasia: Causes, Symptoms & Treatment

Table of Contents
- What is Endometrial Hyperplasia?
- What are the Types of Endometrial Hyperplasia?
- How Common is Endometrial Hyperplasia?
- What Are the Symptoms of Endometrial Hyperplasia?
- What Are the Causes of Endometrial Hyperplasia?
- What Are the Complications of Endometrial Hyperplasia?
- How is Endometrial Hyperplasia Diagnosed?
- What is the Treatment for Endometrial Hyperplasia?
- Bottom Line
Many women experience changes in their menstrual cycle or unusual bleeding at some point, but few realize these can sometimes signal changes in the uterine lining.
One such condition is endometrial hyperplasia, where the lining of the uterus becomes thicker than normal.
While it’s not always serious, it can sometimes lead to complications if left untreated. In this blog, we will understand the various types of endometrial hyperplasia, their causes, and treatment options. Understanding them will help with early diagnosis and better management of the condition to decrease the chances of complications.
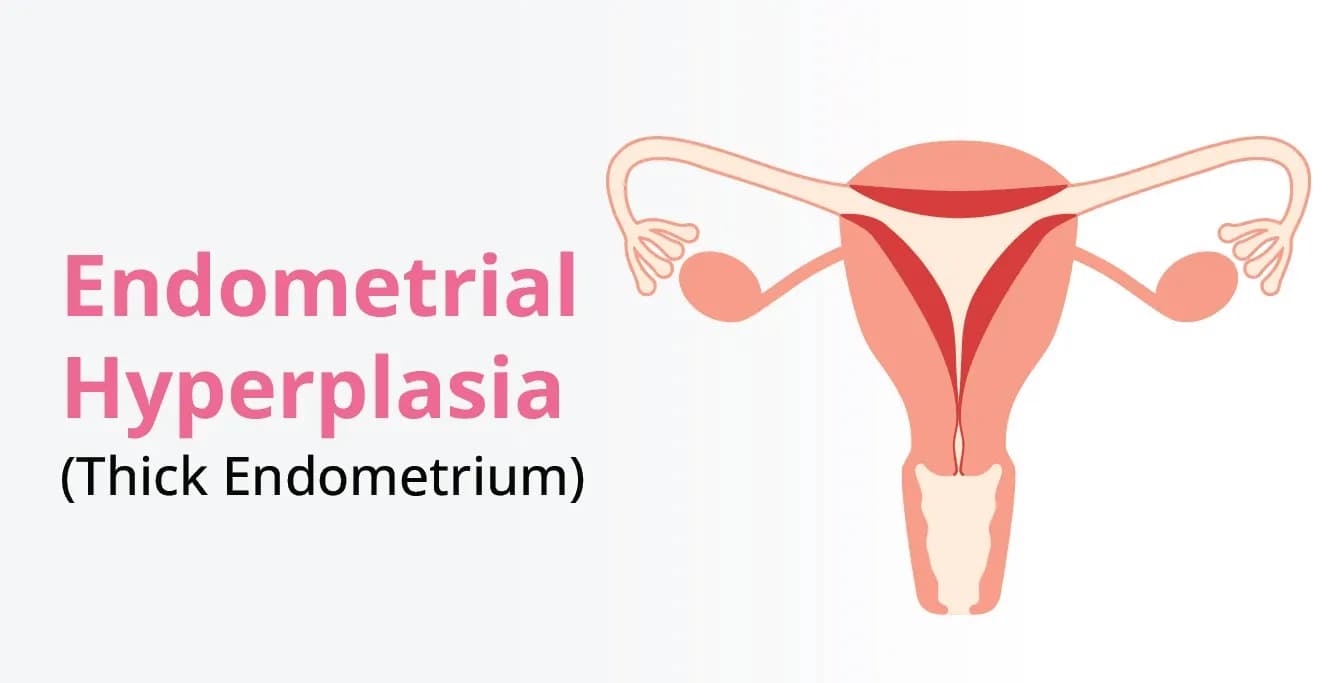
What is Endometrial Hyperplasia?
In women, menstruation and conception both depend on the endometrium. It gets thicker each month in readiness for a possible pregnancy. If no pregnancy happens, it is shed during your menstrual cycle. The normal range for endometrial thickness is 2–16 mm, depending on the menstrual cycle phase, and less than 5 mm after menopause.
At times, this wall (endometrium) becomes abnormally thick, which is called endometrial hyperplasia. The meaning of a thickened endometrium is that the uterine lining grows more than normal, often due to hormonal imbalance, like estrogen (high) and progesterone (low). It is common for women aged 45 and above as they are approaching menopause. Certain factors, like obesity, polycystic ovary syndrome (PCOS), or taking estrogen-only hormone therapy, can also increase the risk.
What are the Types of Endometrial Hyperplasia?
Endometrial hyperplasia comes in a variety of forms, depending on how the cells look and whether or not atypia (abnormal cells) are present. Here are the different types of thickened uterine lining:
- Simple Endometrial Hyperplasia (without atypia): This is the type where the endometrium becomes slightly thicker with mild cell crowding, but the cells look normal. They are generally mild and won’t progress to cancer if treated properly.
- Complex Endometrial Hyperplasia (without atypia): This is a slightly more intense type of endometrial hyperplasia. In this, the gland cells grow more densely and irregularly, but there are still no abnormal cells. When diagnosed on time and properly treated, there is a high chance of the condition improving without the risk of cancer in the future. Though if not treated, it has a low cancer risk.
- Simple Atypical Endometrial Hyperplasia: The lining is thickened, and some gland cells start to appear abnormal under a microscope. This type has a higher chance of turning cancerous if not managed promptly.
- Complex Atypical Endometrial Hyperplasia: This is the most serious type of endometrial hyperplasia, where there are a lot of glands and abnormal cells. As the name suggests, it is very complex and carries the highest risk of developing into endometrial cancer without timely treatment.
How Common is Endometrial Hyperplasia?
Particularly in women going through or approaching menopause, endometrial hyperplasia is a somewhat frequent disorder. Women between the ages of 40 and 55, when hormonal fluctuations are common, are most commonly affected. The disorder is brought on by high estrogen levels that are not balanced by enough progesterone, which causes the uterine lining to develop excessively. Women who use estrogen-only hormone therapy, have diabetes, obesity, or PCOS are more vulnerable. Certain types, particularly those with unusual cells, may worsen if treatment is not received, even though not all cases result in cancer. Better results and efficient care are ensured by early diagnosis.
What Are the Symptoms of Endometrial Hyperplasia?
It can change one’s life to identify the symptoms when they first appear. Typical thickened endometrium symptoms include:
- Heavy periods or bleeding in between cycles are examples of abnormal uterine bleeding.
- Pressure or soreness in the pelvis.
- Irregular menstruation, particularly during menopause.
- Cycles that are abnormally long or short.
- See a gynaecologist right away if you are also having any of these symptoms.
So, if you ever see any of these thickened endometrium symptoms, consult a doctor with similar experience.
What Are the Causes of Endometrial Hyperplasia?
There are mainly two causes behind endometrial hyperplasia. Here they are:
Hormonal Imbalance
As we already mentioned above, hormonal imbalance between estrogen and progesterone is the most common reason for endometrial thickness. On the one hand, estrogen helps the endometrial lining to grow so that it can help with the conceiving and pregnancy process; on the other hand, progesterone keeps this growth in check and triggers the shedding every month, which we call the menstruation cycle.
When the body produces too much estrogen but not enough progesterone, the lining of the uterus can become thicker than it generally should be. Irregular periods can happen, and over time, this can lead to an abnormal buildup of endometrial tissue, also called endometrial hyperplasia.
Risk Factors
Certain conditions and lifestyle factors can increase the likelihood of developing endometrial hyperplasia. These include:
- Obesity– Higher body fat increases estrogen levels, disrupting hormonal balance.
- Polycystic Ovary Syndrome (PCOS)- Women with irregular ovulation experience prolonged estrogen exposure.
- Menopause– Women aged 45 and above who are approaching menopause can have hormonal fluctuations, which create an imbalance.
- Diabetes- Linked with insulin resistance, which may influence hormone production.
- Hormone Therapy- Long-term use of estrogen without progesterone (such as in some hormone replacement therapies) can raise the risk.
Understanding the causes and risk factors helps with early detection and prevention. It also helps you take proactive steps to maintain hormonal balance and uterine health without having any future complications.
What Are the Complications of Endometrial Hyperplasia?
Now that you have understood the various reasons for endometrial thickness, here are the possible complications that can happen if left untreated:
- Increased Risk of Endometrial Cancer– There is a high chance that cases with atypical cells could lead to complications in the future. It is especially true for cases where diagnosis or treatment is not done on time. These abnormal cells can grow and progress to uterine or endometrial cancer.
- Heavy Bleeding– The thickened uterine lining can cause heavy and irregular periods for an extended period. This not only leads to discomfort but can also affect the daily life routine.
- Anemia- This is a condition in which hemoglobin levels are low. Chronic heavy bleeding can result in anemia that can cause weakness, fatigue, and dizziness because of low red blood cell count.
- Fertility Issues- A thickened endometrial lining can interfere with embryo implantation, making it difficult to conceive naturally.
- Emotional Impact- Dealing with abnormal bleeding or cancer risk can cause anxiety and stress, affecting overall well-being and quality of life.
How is Endometrial Hyperplasia Diagnosed?
Many conditions can cause abnormal uterine bleeding. To identify what’s causing your symptoms, your healthcare provider may order one or more of these tests:
- Ultrasound– A transvaginal ultrasound uses sound waves to produce images of your uterus. The images can show if your uterine lining is too thick.
- Biopsy– An endometrial biopsy removes tissue samples from your uterine lining. Pathologists study the cells under a microscope to confirm or rule out cancer.
- Hysteroscopy– Your provider uses a thin, lighted tool called a hysteroscope to examine your cervix and look inside your uterus. Your provider may perform this procedure along with a dilation and curettage (D&C) or biopsy. With hysteroscopy, your provider can see abnormalities within the endometrial cavity and take a biopsy of any suspicious areas.
What is the Treatment for Endometrial Hyperplasia?
The treatment of endometrial hyperplasia (thick endometrium) depends on the type and severity. Endometrial thickness treatment includes:
| Treatment Type | Description |
| Hormonal Therapy | Progestin therapy is commonly used to balance estrogen levels and reduce the thickness of the endometrial lining. |
| Dilation and Curettage (D&C) | A surgical procedure that involves scraping and removing the abnormal tissue from the uterine lining. |
| Hysterectomy | In severe cases or for women who have completed their family planning, a hysterectomy may be recommended, which involves the removal of the uterus. |
Bottom Line
Endometrial hyperplasia is a condition where the uterine lining develops abnormally due to a hormonal imbalance. Even though it might be frightening, especially when atypia is present, it is typically treatable with prompt action.
Whether you have cystic endometrial hyperplasia, are undergoing treatment for endometrial hyperplasia, or simply want to understand your risk factors, being informed is the first step towards better health.
Our Fertility Specialists
Related Blogs
To know more
Birla Fertility & IVF aims at transforming the future of fertility globally, through outstanding clinical outcomes, research, innovation and compassionate care.
Had an IVF Failure?
Talk to our fertility experts

 Our Centers
Our Centers